Kidney health is key to our overall wellbeing. Healthcare professionals use a measurement known as the Glomerular Filtration Rate (GFR) to monitor how well our kidneys are working to clean our blood.
Glomeruli are tiny filters in our kidneys that help remove toxins from our blood. The GFR measures how much blood these filters can clean every minute. Monitoring our GFR helps doctors keep an eye out for the onset of kidney disease – the major disease of concern being Chronic Kidney Disease (CDK) – and provide the right degree of individualized treatment, ranging from advice on simple lifestyle changes through to kidney transplant or dialysis.
However it can’t be measured directly. The calculation is complex, based on multiple factors like age, body size, sex, race/ethnicity, as well as the level of creatinine – a waste product – in the blood.
Pharmacists strive to avoid the risks associated with the progression of kidney disease, of overdosing or underdosing – indeed any factors that potentially hinder optimal delivery of treatments and the patient’s recovery. Accurate calculation of GFR and CrCl are therefore vital to minimizing risks to patients.
The Challenges of Measuring CrCl and GFR
The GFR reveals the rate at which fluid is filtered by the kidneys, while creatinine clearance, CrCl, measure how much creatinine is in your blood. Healthy kidneys filter it out, but if you have kidney disease, creatinine stays in the blood and gradually builds up.
Creatinine levels and GFR are both measured by using creatinine samples from serum or urine. Creatinine collected from one source can be compared with creatinine from the other source. For comparison purposes, serum collection has to be within 24 hours of urine collection and vice versa. Serum creatinine samples are typically collected more than urine samples.
Healthcare professionals need the CrCl calculations in order to provide the estimated GFR – as GFR is not measured directly in practice. But despite the fact that CrCl calculations are performed commonly, GFR calculation is not error free. CrCl overestimates GFR by 10-20%. This is due to creatinine being freely filtered by the glomerulus while also being secreted by the capillaries.
Further challenges to measuring creatinine clearance involve improper urine collection. This leads to an underestimation of creatinine excretion. Age-related increases in tubular secretion result in overestimation of GFR.
Other challenges include sex and race, with specific factors affecting creatinine production and clearance.
The Challenges of Calculating Drug Dosages
The difficulty here is that healthcare professionals need to complete a thorough examination of the patient’s history. Knowing and understanding the patient’s chief complaint, the history of the current illness, their prior medical history, social history, family history, medication, and prior treatments is all crucial to deciding which types of medication can be prescribed and at what dose.
To sum it up, every patient is different. There is no “one size fits all” treatment option. Fortunately there are practice guidelines that can be referenced, but these still have to be tailored to best suit the patient. Many factors play a part. One important factor, for example, outside of guideline recommendations and best practices, is patient preference. Healthcare professionals need to be aware that just because a reliable source suggests a particular method this does not mean it will always be successful.
What Do the Numbers Mean?
High serum creatinine levels and low creatinine clearance indicate abnormal renal (kidney) function.
A normal creatinine clearance level for healthy women is 100-130mL/min or 110-150 mL/min for men. People whose kidneys are functioning normally will have a serum creatinine level 0.5 and 1.1mg/dl for women or 0.6 to 1.2 mg/dl for men.
How Are the Numbers Calculated?
As we already mentioned, CrCl is measured by monitoring creatinine levels. We use the Cockcroft-Gault formula, which includes a patient’s weight (kg), age and gender, to estimate CrCl in mg/dL.
For GFR, there are several formulas you can use:
- Modification of Diet in Renal Disease Study Group (MDRD) – includes serum creatinine, age, ethnicity, and albumin levels. Recommended for detecting a GFR lower than 60 mL per minute or lower than 90 mL in older patients.
- Chronic Kidney Disease Epidemiology Collaboration (CKD-EPI) – based on gender and whether a patient is black or non-black. Practice guidelines recommend this formula for the estimation of GFR.
- Mayo Quadratic formula – used to better estimate GFR in patients that have preserved renal function
- Schwartz formula – estimation of GFR in children
Free Up Valuable Time with Automated, On-the-Fly Calculations
Easily accessible automation is one of the main reasons why we think KNIME is a good platform for Creatinine Clearance, Glomerular Filtration Rate and Drug Dosage Calculations.
I have used KNIME to build calculators that can be used in a clinical setting. They have the potential to free up a healthcare professional’s time – bypassing the need to look up appropriate calculation formulas, nephrotoxic medications, and dosing guidelines.
With my interactive calculator everything the healthcare professional needs is available in one place. It provides the means to calculate the gold standard calculation of creatinine clearance, gives you the normal ranges for men and women, enabling you to refer and check your calculations.
The calculator also adds in the ability to make your calculations more precise with two further methods of CrCl calculation depending on whether the patient is at home or hospitalized.
Tip: Download the workflow behind the data app from the KNIME Hub
KNIME, as a code-free data analytics platform, and a powerful one at that, opens up access to advanced analytics to the subject-matter experts. Now, we healthcare professionals can also build customized workflows suited to our specific needs in the clinic. N prior coding knowledge is necessary to use KNIME!
Take it from me, a fourth-year pharmacy student with minimal programming knowledge is now a third level certified KNIME user- It took 1-2 weeks to gain my certification in using KNIME; within, 3 weeks I was comfortable with application practices. I have learned KNIME concepts and utilization for my five-week advanced pharmacy practice experience (APPE) digital health rotation. KNIME provides its users with many tools, and even has the capability to incorporate outside functionality when the integrated tools are not enough. The community too is steadily growing, broadening the possibilities of what KNIME can do, across various practice settings.
The Magic Under the Calculator’s Hood: The KNIME Workflow
My workflow consists of four main components to calculate Estimated CrCl, Modified CrCl, Direct CrCl, GFR & Drug Dosage. Each component is then made up of many different nodes and widgets that coexist to create the completed interactive calculators, accessible via the KNIME web portal.
Below you will find an example of what the inside of each component looks like, give or take.
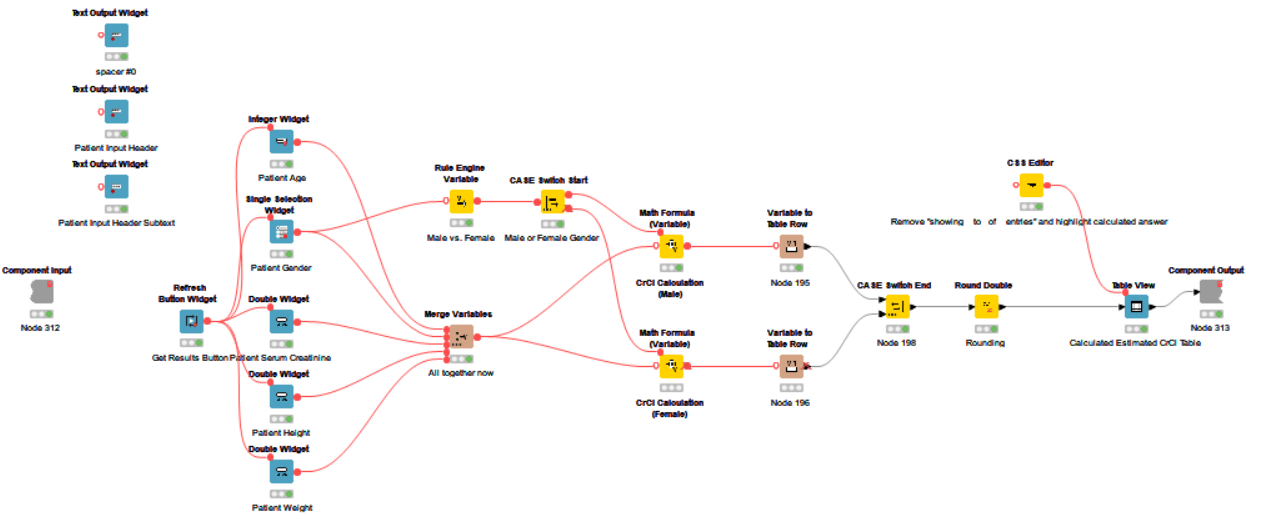
Widget nodes (blue) create how the interactive part of the calculator will look, math formula nodes carry out the calculations and numbering aspects (yellow), and variable nodes mark what data is to be used (brown).
Interactive Data App for Estimated CrCl Calculation
When everything is placed together as desired, complete with instructions, you have an interactive tool to utilize at your command.
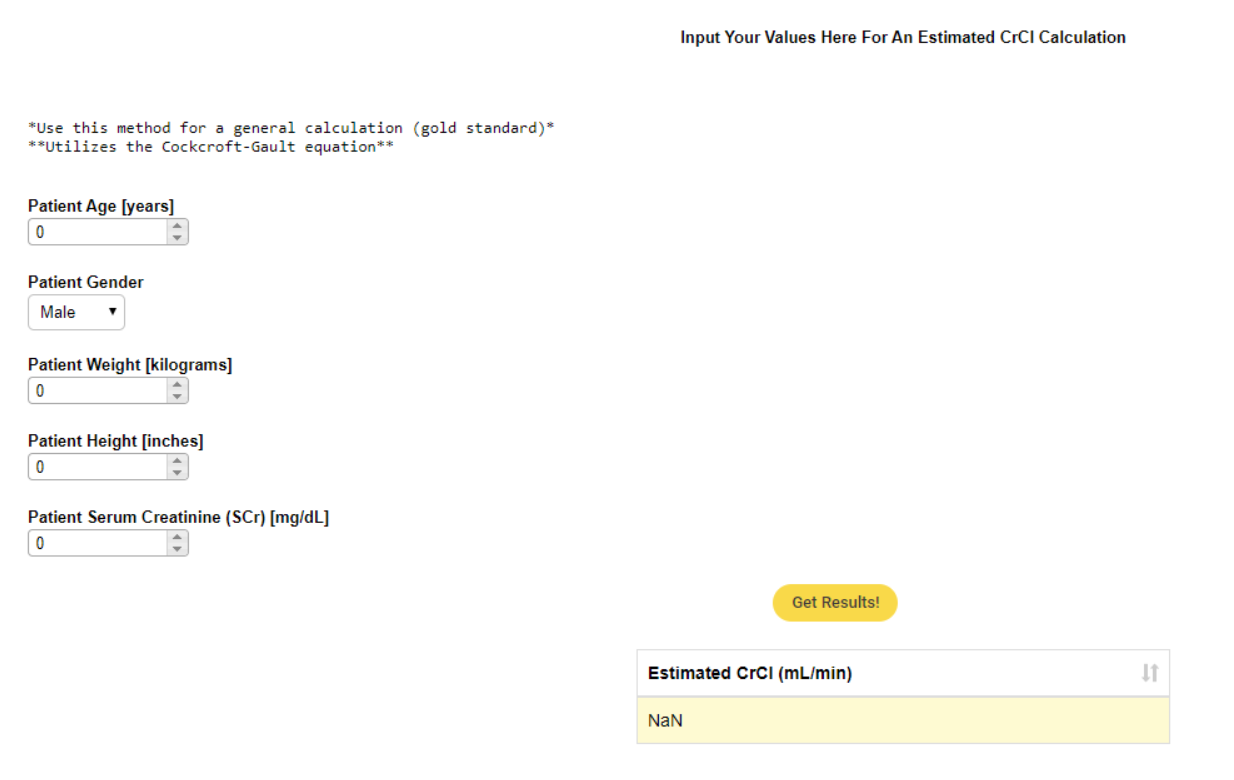
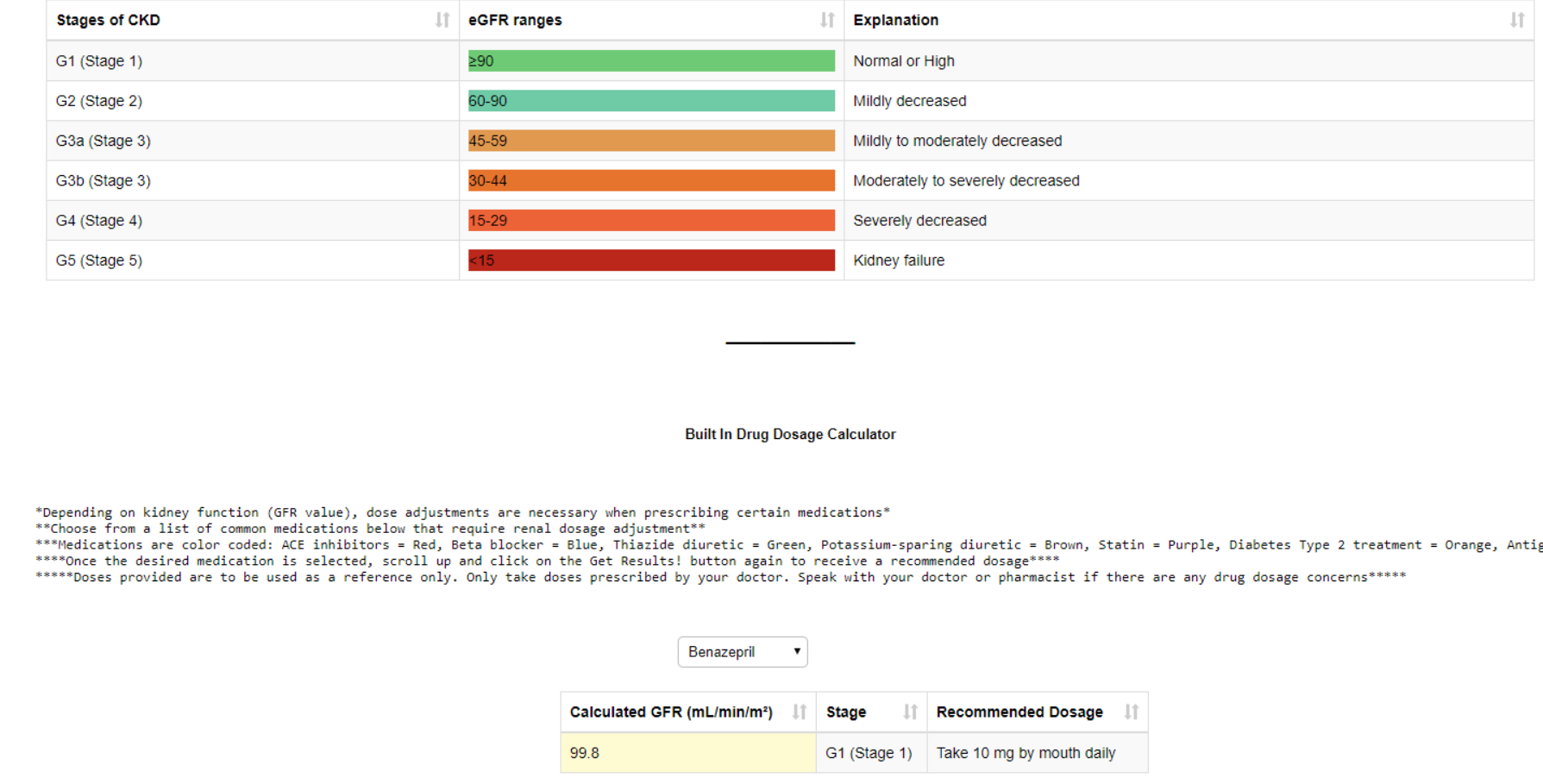
5 Weeks from Project Start to Project Finish
My short term goal was, as the first digital health student to have L3 certification, to have my completed interactive calculator live on the digital health KNIME Server, accessible via the KNIME hub for others to use. Check!
Next Steps: Connect Data App to Lexicomp Drug Database
My next steps now are to make updated versions of the calculator, adding more input options, to work towards achieving my overall desire to connect the calculator to Lexicomp’s drug database. This achievement would allow vast selection and appropriate dosing of many medications, far more than what is available now.
